Reduce Scoliosis without surgery
Tell us your goals and we’ll customize a program that will keep you ahead of the curve. It’s free, and it only takes 60 seconds.
From our Blog
Scoliosis, a lateral curvature of the spine, is a condition that affects individuals across their lifespan, presenting unique challenges at different stages...
The human spine is a complex and vital structure that provides support and flexibility to the body. However, various conditions can affect...
Scoliosis, a condition characterized by an abnormal curvature of the spine, often prompts individuals to explore various forms of exercise to manage...
Case Studies
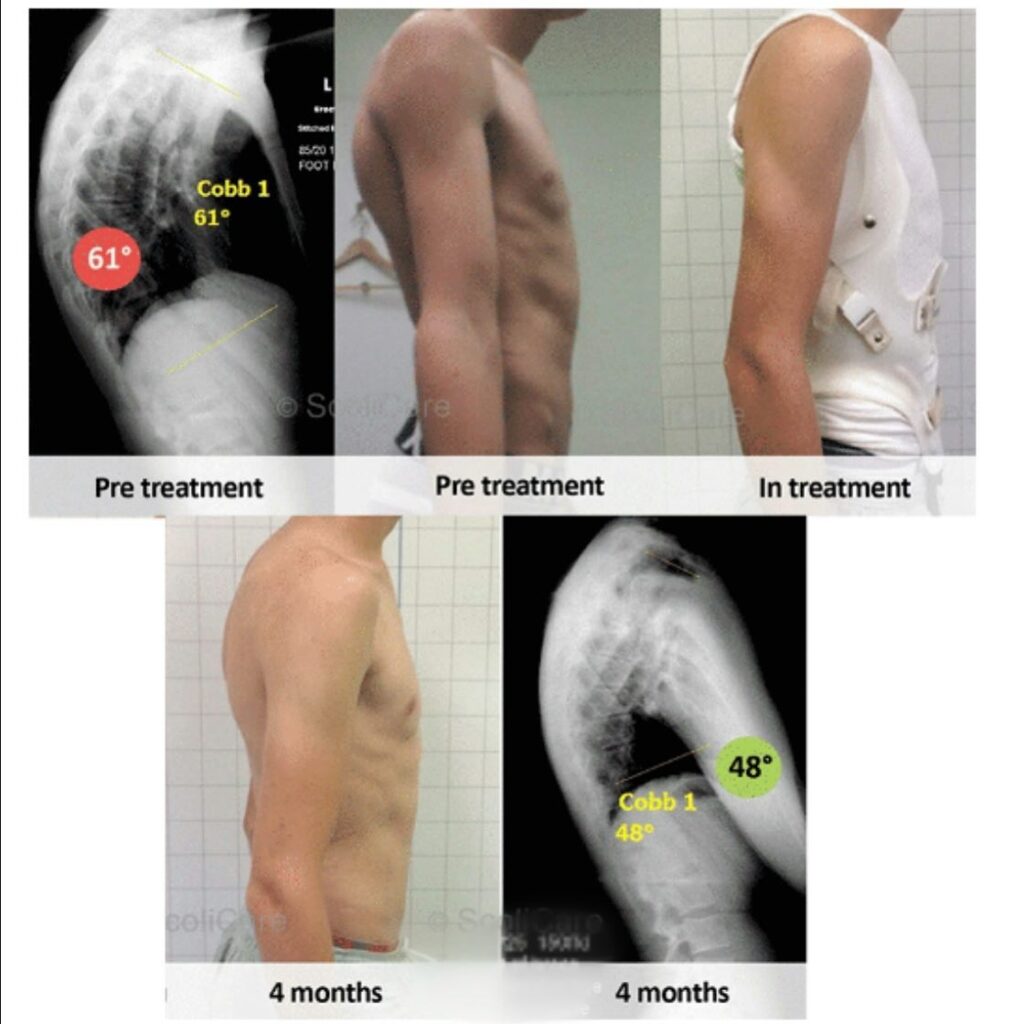
Case Study 11
This is a case of Kyphosis – excessive outward curvature of the spine, causing hunching of the back. 61° (hyper kyphosis) reduced to 48° (normal amount of kyphosis).
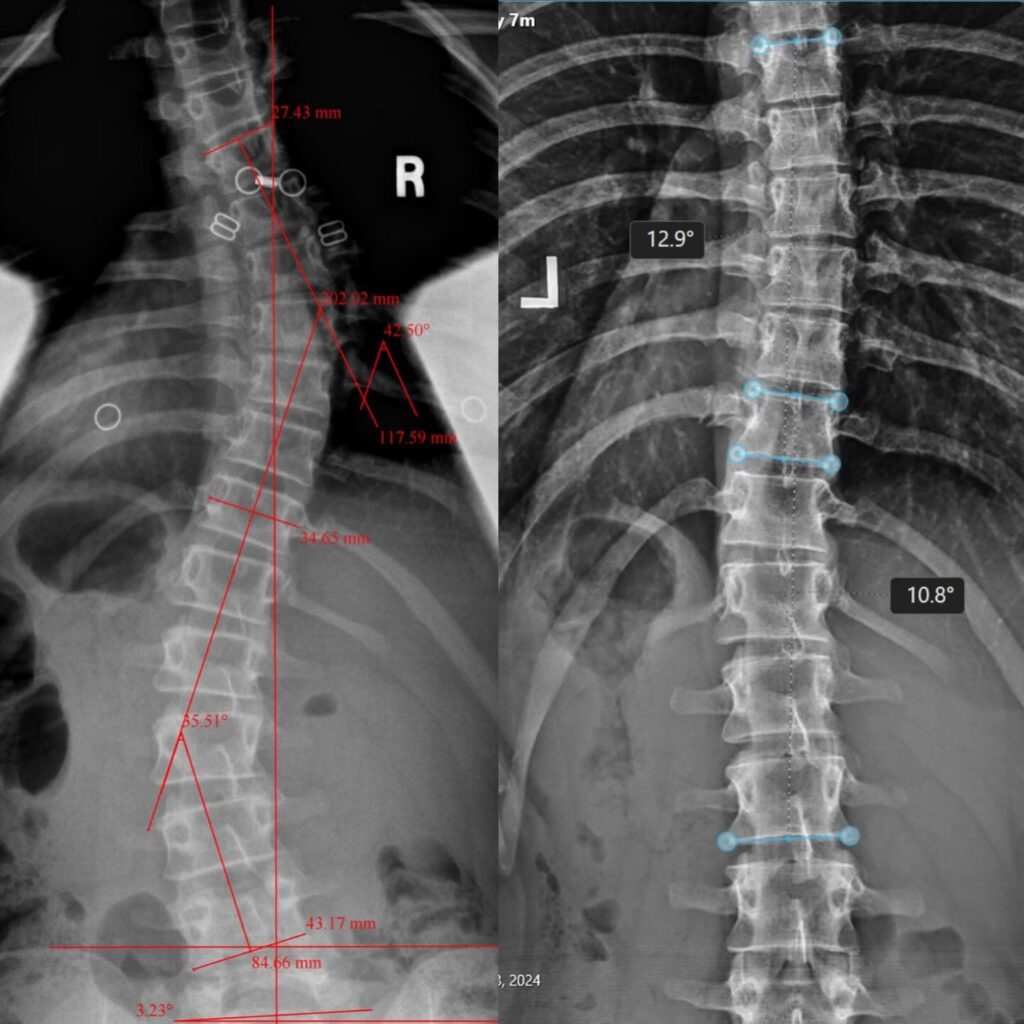
Case Study 19
BEFORE & AFTER 42.5°/35.5° down to 12.9°/10.8°.
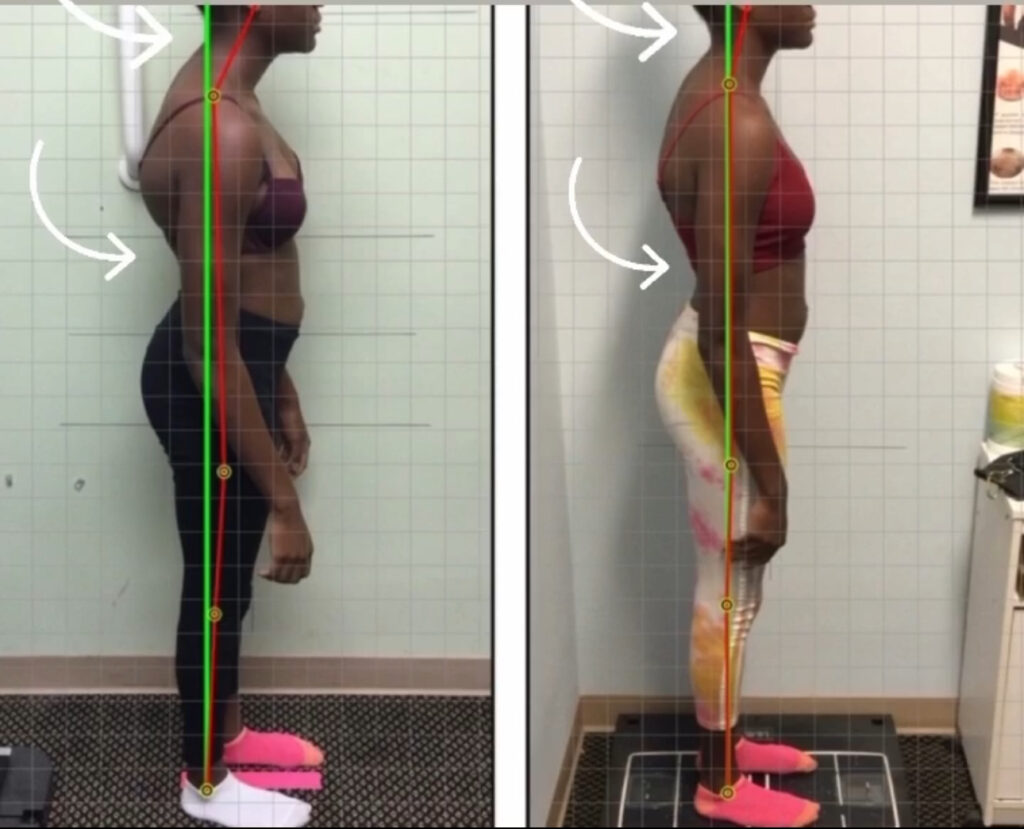
Case Study 6
14-year-old female patient came to us with severe kyphosis causing noticeable cosmetic abnormality. As seen in the right photo, patient shows significant postural change after just one week of treatment #straussmethod (exercise and therapy only, no bracing).
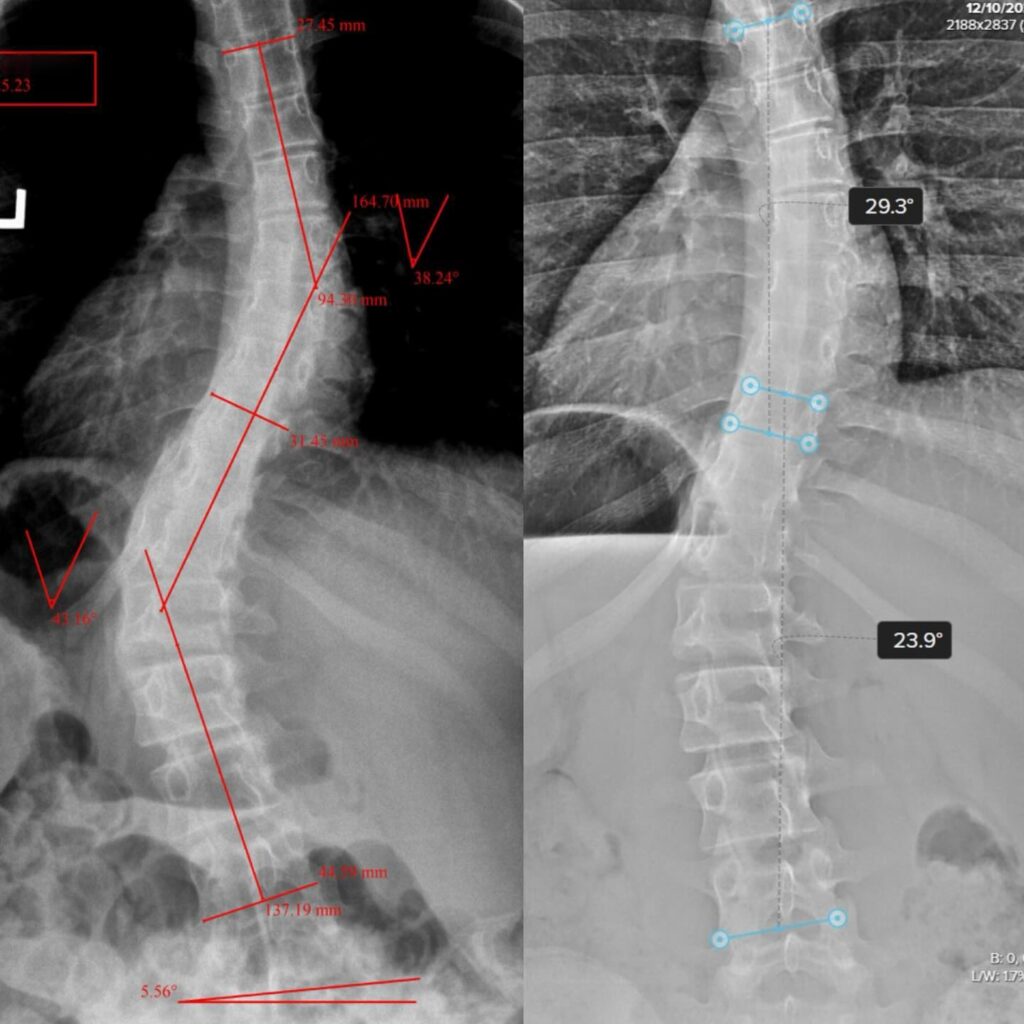
Case Study 18
38°/43° down to 29°/23°.
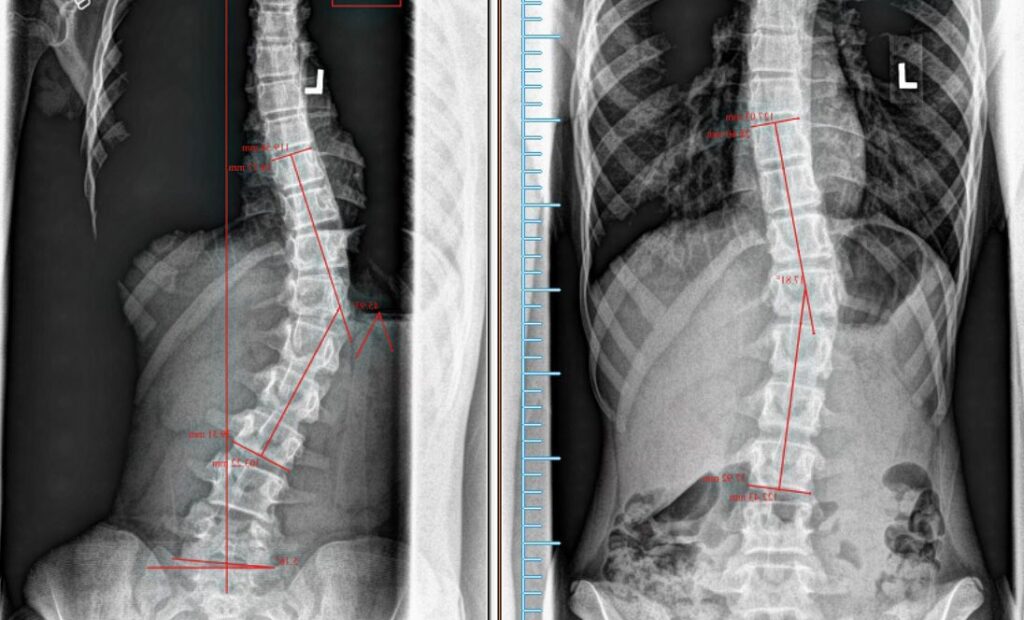
Case Study 1A
Patient began care at 12 years old.
Severe surgical level curve of 46° reduced to 17° over 2 years of care.
Family rejected the surgical option.
2 years after care and her corrections are stable.
Our goal: Avoid surgery!
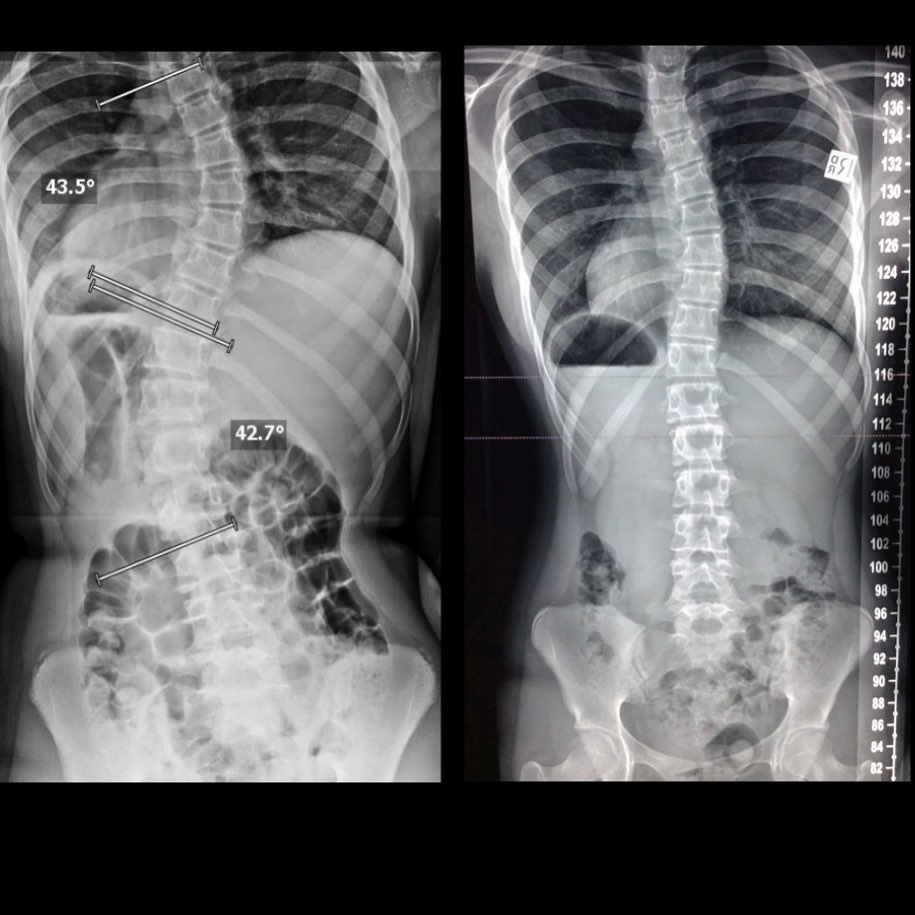
Case Study 15
Incredible results after 26 months. Custom designed scoliosis specific home exercises, ScoliBrace, along with specific chiropractic alignments and therapy.
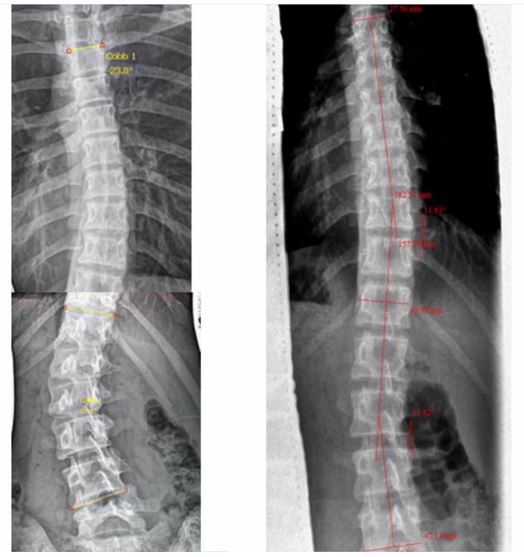
Case Study 12
All LARGE curves started as small curves. Scoliosis is much easier to treat when the curves are small!
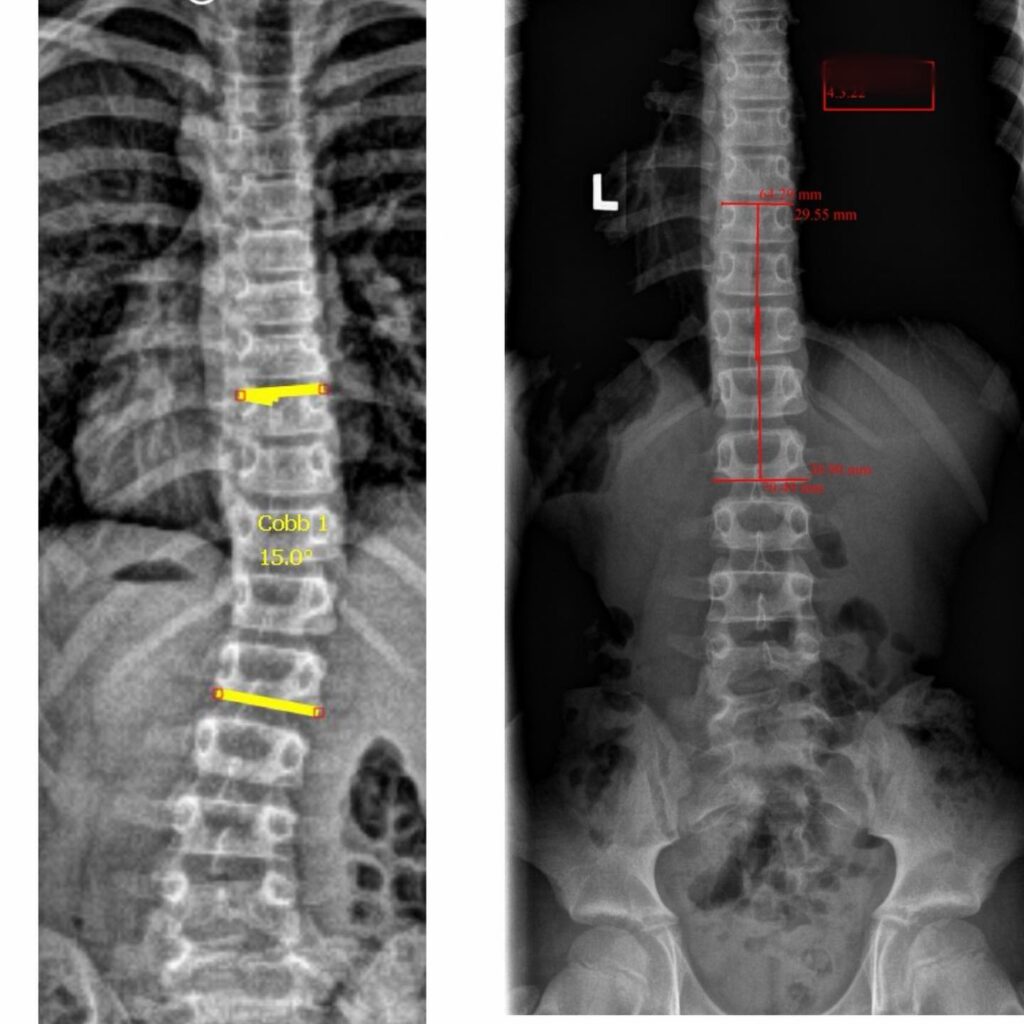
Case Study 8
15° to 0° in a 9 year old!!
Since the father of this patient has very large curve, the parents were very concerned and noticed a mild curve early. As we always say, every LARGE cure was once a small curve, and small curves are much easier to treat.

Case Study 16
The typical approach to treating mild scoliosis in children is simply to “watch and wait”- and see how the curve progresses. But most juvenile scoliosis curves are at high risk of worsening without treatment. The good news? Scientific studies have shown that individually designed, nonsurgical treatment programs can halt progression and even reduce scoliosis curves.
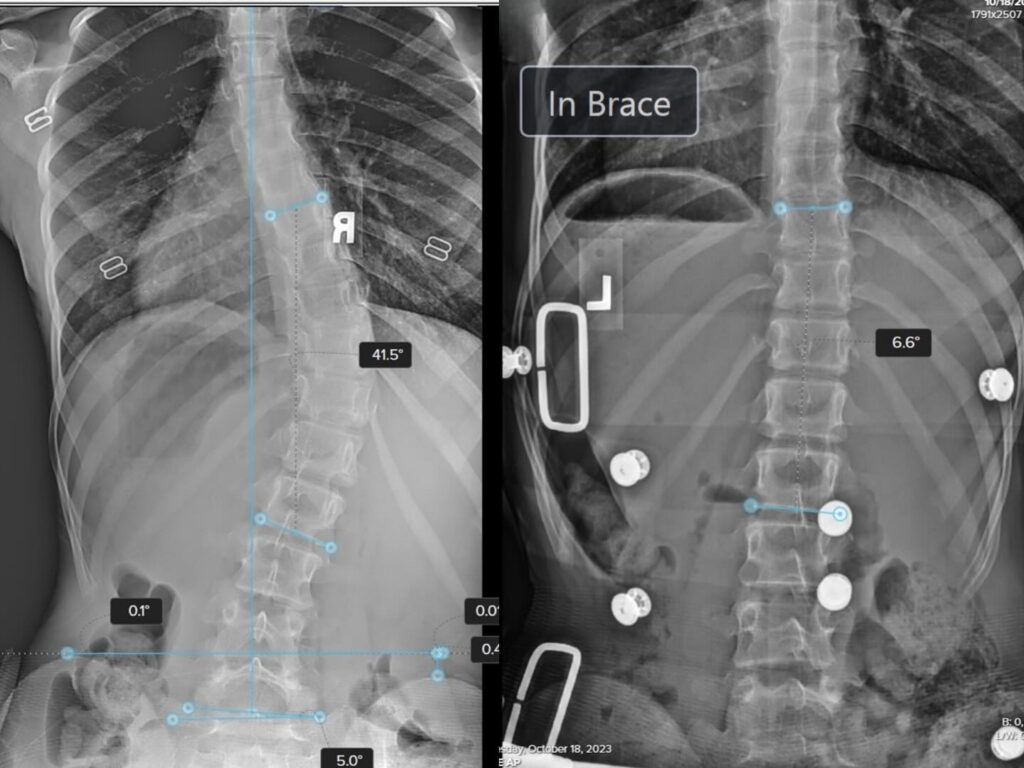
Case Study 17
Incredible in-brace correction with ScoliBrace. We select from 7 different braces to get the best fit for the patient.
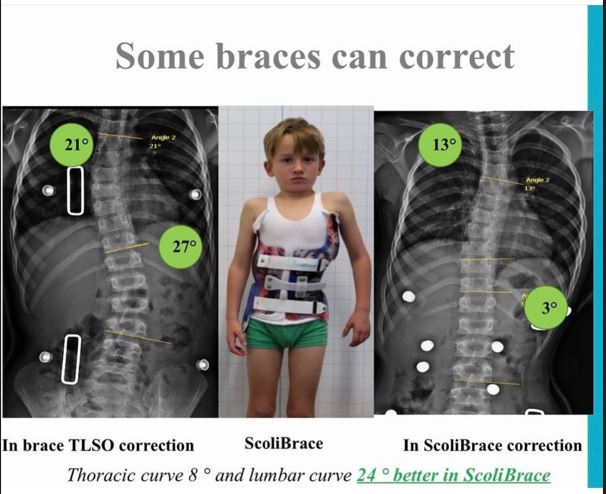
Case Study 10
NOT ALL BRACES ARE THE SAME!! We see so many patients in our office that come in with braces that have minimal correction. We offer LASER scan precision in design plus in-house brace modifications for the best initial fit AND brace modifications during the course of treatment to provide the best continuing correction as the spine is straightening.
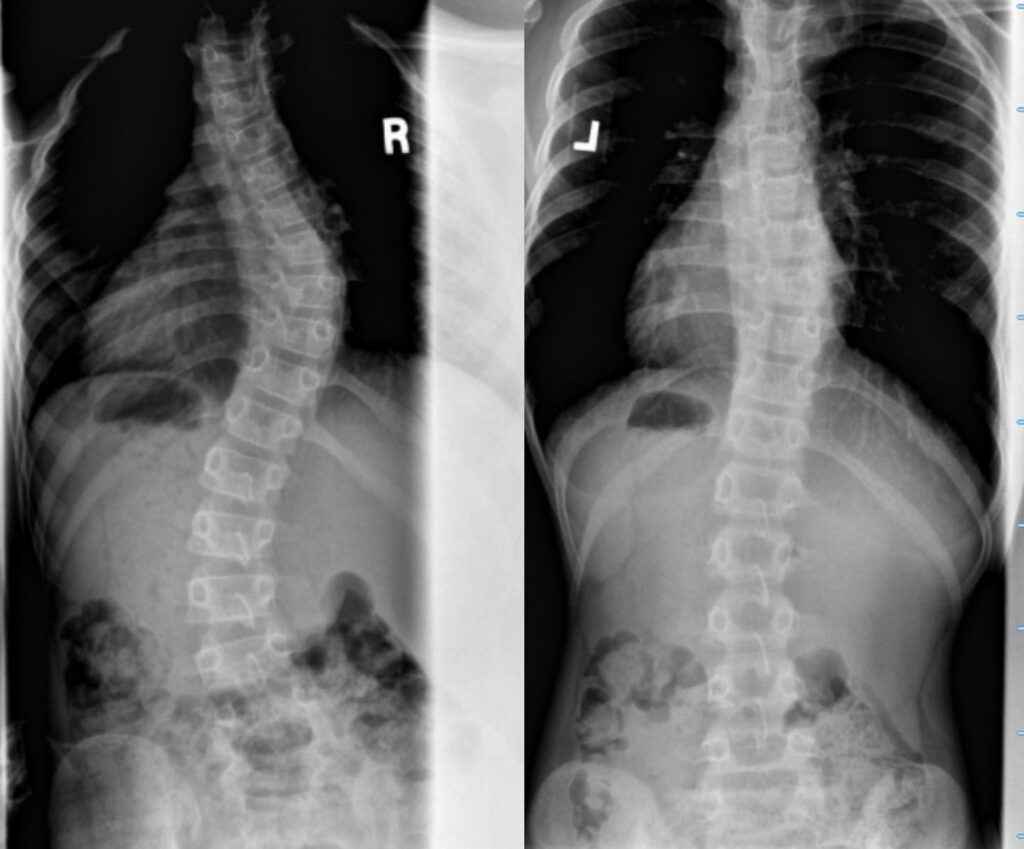
Case Study 3
Juvenile Idiopathic Scoliosis.
46° curve reduced to 20° degrees in a 7 year old male,
Juvenile scoliosis can be a dangerous and progressive form of scoliosis due to amount of growth the child will experience!
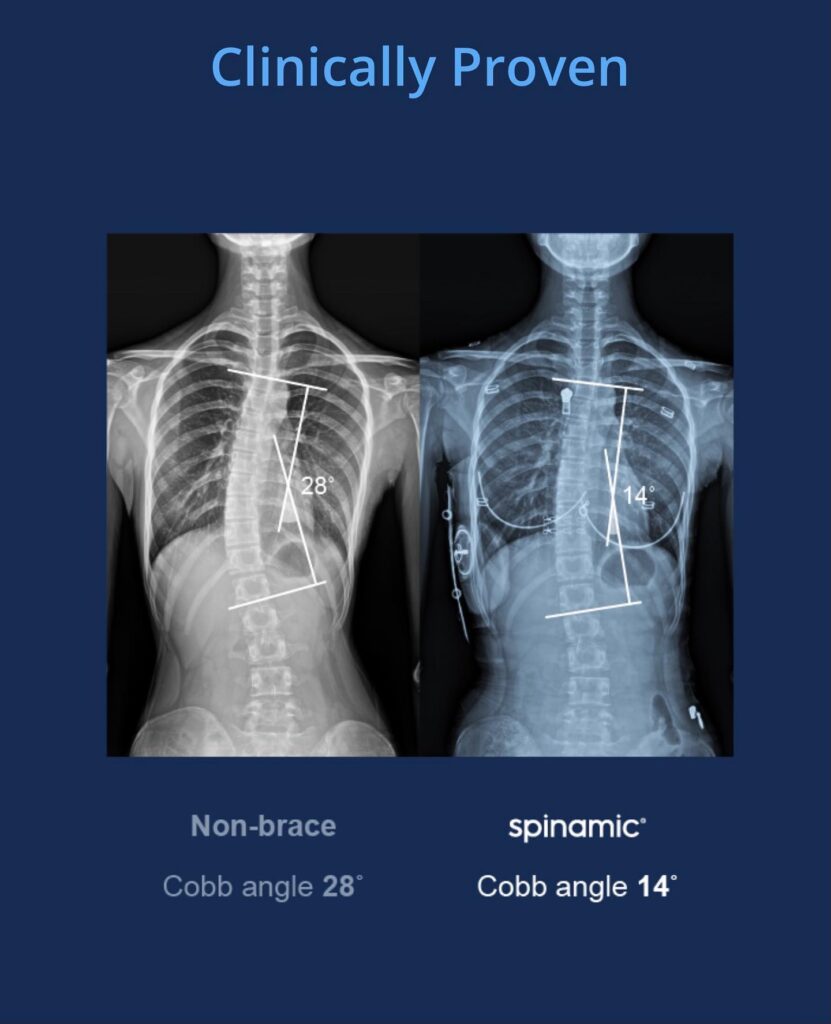
Case Study 9
The Spinamic Brace is a hybrid soft jacket based system clinically proven to significantly correct mild to moderate, flexible curves.
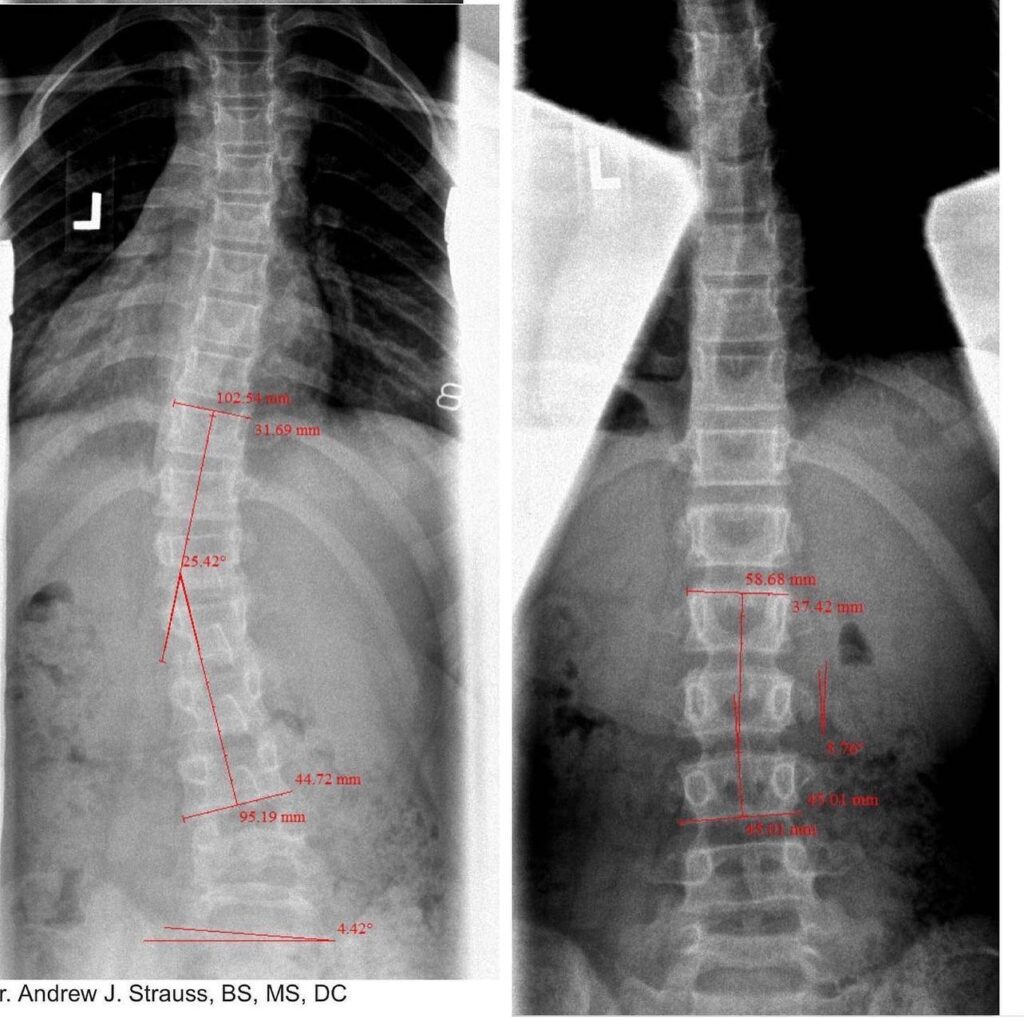
Case Study 2
A 25° scoliosis reduced to 5°with the straussmethod.
Custom designed scoliosis specific home exercises along with a selection of specific chiropractic, yoga for scoliosis, instruction in activities of daily living, targeted stretching, active self-correction, and nutritional advice, plus the addition of the most advanced bracing options if necessary.
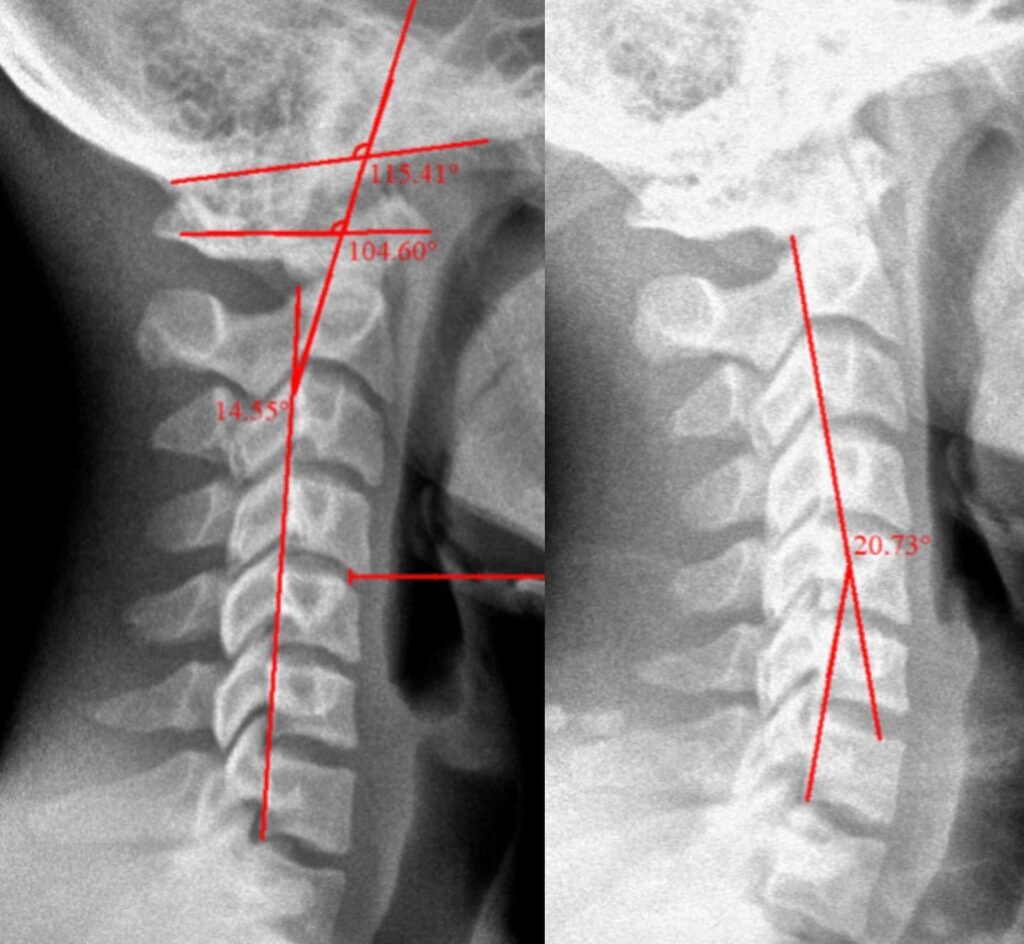
Case Study 4
Restoration of the normal spinal curves is essential!
This patient had a reversal of the normal neck curve.
The reversal is corrected with application of appropriate home exercise, spinal molding, and postural education.
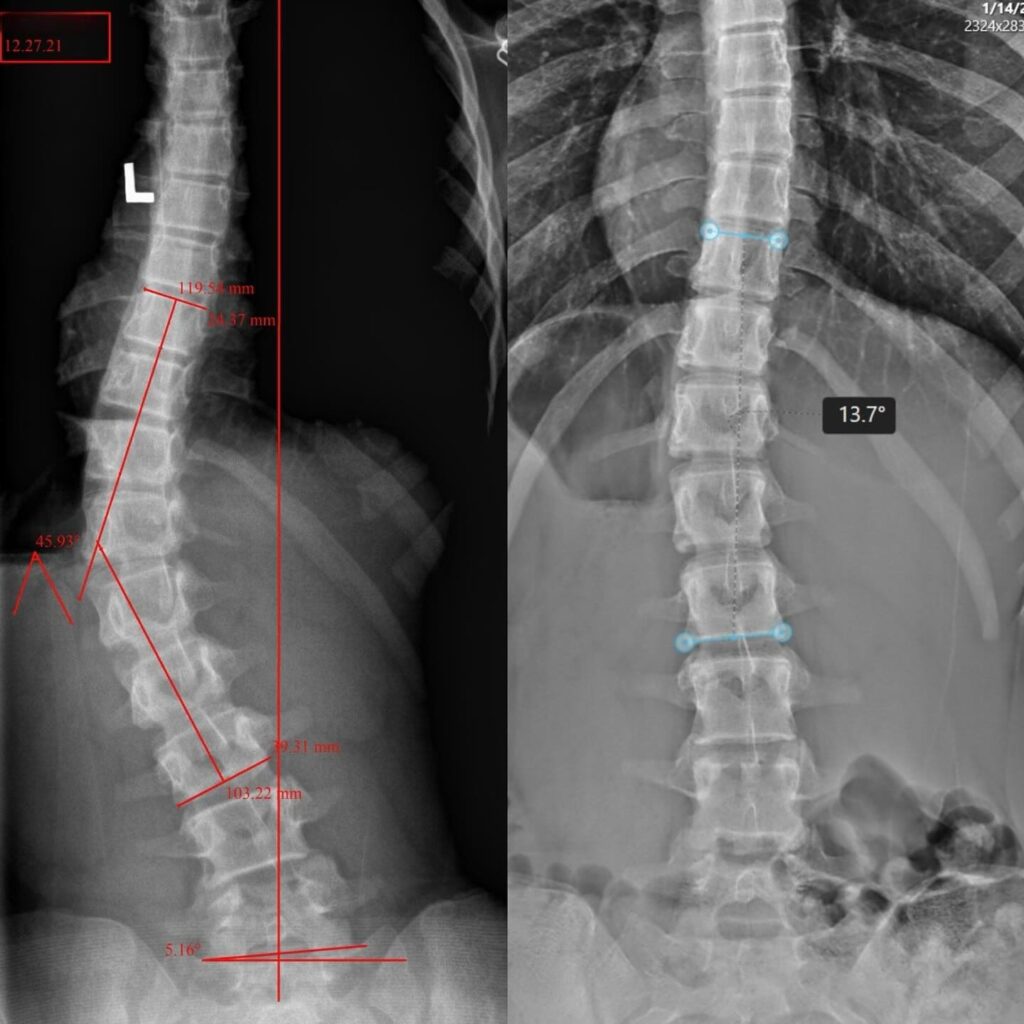
Case Study 20
BEFORE & AFTER
42.5°/35.5° reduced to 12.9°/10.8°
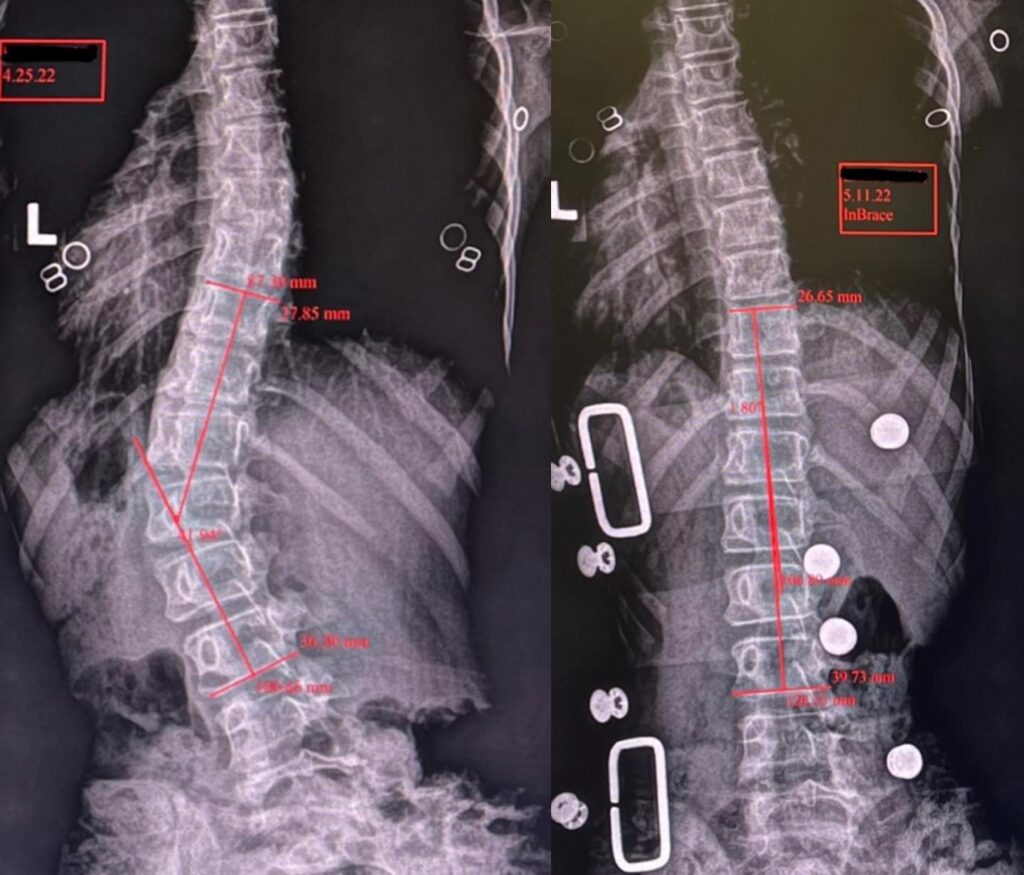
Case Study 7
In-brace X-ray shows a slight overcorrection which is an ideal bracing response! In brace X-ray is used to predict response to care. Scoliosis corrected in brace from 42° down to -2°.
Play Video
Meet Dr. Andrew Strauss
For over thirty-nine years, Dr. Strauss has relieved the pain and improved the quality of life for thousands of scoliosis patients who sought relief without surgery. The Strauss Method is a unique combination of the most advanced research-based
scoliosis treatments, customized by Dr. Strauss for each patient.
Keeping scoliosis patients ahead of the curve
The typical approach to treating scoliosis is to “watch and wait”—and see how the curve progresses. But studies have shown that individually designed, nonsurgical treatment programs can stabilize and even reduce scoliosis curves. And the sooner you treat your curve, the more effectively you’ll be able to halt its progression.

In pain? Treat the cause, not just the symptoms
Scoliosis pain is rare in children, but it’s common in adults. In fact, up to 92% of adults with scoliosis experience pain as a result of their condition. Fortunately, you don’t have to suffer. But you do need to treat the cause and not just the symptoms of scoliosis pain.
Which treatment plan is right for you?
Tell us your goals and we’ll customize a program that will keep you ahead of the curve. Get started for free today. It only takes 60 seconds.

The Truth About Adult Scoliosis: What You Need to Know About History, Treatment Options, and How to Prevent Progression
By Dr. Andrew Strauss
What our patients are saying
At Strauss Scoliosis Correction, we’ve helped over 10,000 scoliosis patients eliminate pain and stabilize their curves. Here’s what they have to say about their treatment.
I searched Google and found out about Dr. Strauss’s method of treatment. We decided to see Dr. Strauss because, in France, we don’t have intensive treatment and this equipment.
We tried Kinesitherapy in France, osteopaths, swimming. They wanted to go faster and they hurt Nicolas. Dr. Strauss takes care so the patient has no pain and the equipment is very appropriate with exercises and special equipment to correct scoliosis.
Nicolas has a serious scoliosis and it is a long road ahead. We know Nicolas has a strong scoliosis and it’s hard work but we don’t give up and we see improvements.
Thank you Doctor Strauss!

Mrs F., mother of Nicolas F., age 16, and Gabriel F., age 14, France
We had a good impression from the reviews we read. We chose Hudson Valley Scoliosis because it offers new alternatives to treat scoliosis. We liked everything about your center.
We were very satisfied. Usually Sami does not like hospitals or doctors, but this time it was different. He wants to spend more time at your center. The staff is very friendly. Dr Strauss is a wonderful and professional doctor.
Consider Hudson valley Scoliosis before making any decision about surgery or bracing. This center will teach you a lot about scoliosis. Other doctors just tell you to wait and watch which is a big lie.

Mr D., father of Sami D., age 14, Ohio
We hoped to improve our daughter, and we felt this was our only hope. The center was very nice and friendly and Dr. Strauss is a real nice guy. Yasmine really likes him. This is Yasmine’s 2nd round and she likes how everyone here treats her like family.
After returning for our follow up (4 months later) and seeing good results, we know its worth the trip. The only thing I would like to see is a place like this in Ontario. We need a place like this.
We would tell people to come here and try this out before surgery. We DID tell people how we are happy with Dr. Strauss.
Mrs S., mother of Yasmine S., age 14, Ontario
I am a MD, I myself noticed first that my daughter had a scoliosis. I took her to many ortho-spine specialist doctors, and all did nothing. Just wait and observe. I found this center on the internet and researched about it and finally made an appointment.
I am 100% satisfied with Dr. Strauss and his team, and the customized approach of treatment for each different type of scoliosis. I really thank Dr. Strauss and all his team. They are too good, caring, professional…whatever I write for Dr. Strauss & team is less! Amazing people doing a good job. Almighty bless you all!
Please do not go for surgery, what ever type of curve you have, it can be brought down by Dr. Strauss. Just try to visit Dr. Strauss and get it corrected. Surgery is not at all needed unless the curvature is making problems for the internal organs.
Dr A, father of R, age 14, Saudi Arabia
The improvement I experienced the first time I was here prompted me to come back again. Very Satisfied. All staff and Dr Strauss are professional and caring and go out of their way to make the experience as comfortable as possible.
After treatment, when back home, I am so pleased that I am able to send photos to Dr Strauss and receive feedback. I consider this a huge benefit.
I had always been led to believe that my scoliosis would continue to progress as I aged and eventually I would have no other choice than surgery. Dr Strauss has changed all this for me. My scoliosis has improved more than I thought was possible. I am able to manage my scoliosis much better with the home programme. I am not in pain and psychologically, I no longer find the scoliosis as terrifying as I did before. Finding Hudson Valley Scoliosis has been an enormous blessing!

Mandy M., South Africa
I didn’t want to go through scoliosis surgery and so investigated alternative treatment options. Hudson Valley Scoliosis happened to be close to my home.
I am very satisfied. Everybody was pleasant and cordial. Dr. Strauss was able to answer all my questions. What is important to me, is that I learn as much as I can about my own body and receive individually-based treatment.
Do your research. Surgery is only justified in a few extreme cases, has high rates of complication, and does not guarantee improvement. If you are a teenager with scoliosis, be sure to wear your brace, if you have one, and do your CLEAR exercises. As someone who didn’t learn about these until his 20s, let me tell you that chronic physical pain is not something I would recommend–preventive healthcare is always, always your best option.
Richard W.